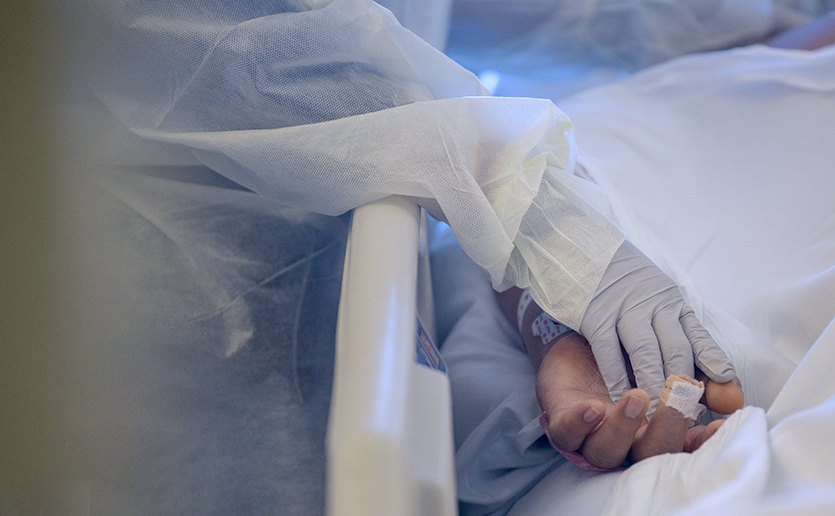
As an emergency medicine physician, Renee N. Salas, MD, MPH, MS, knows the importance of compassionate care. But what happens when personal protective equipment makes human connection difficult? Here, Dr. Salas explains why there’s never been a better time to extend a hand in comfort.
Perhaps one of the most critical skills of an emergency medicine physician is the ability to instantly form connection and trust with strangers, while also rapidly determining the medical issues that require attention. Yet, as with so many aspects of our lives, the COVID-19 pandemic is creating upheaval in these practices while simultaneously bringing clarity to what is important.
Every practitioner has been forced to navigate how and when to be physically present with the patient in the room and when to reach out a hand in comfort.
The vital ritual of donning my protective armor has become second nature: the reused, sterilized N95 mask, protective glasses, gown, gloves and a cap to cover my hair. But patients and colleagues are also wearing masks, which creates an environment where I strain to read emotional states through only small visible facial cues.
Recently, a patient visited the emergency department (ED) for her third time in a week, as she continued to battle her COVID-19 symptoms at home. Her exam and test results continued to look reassuring, and she still did not meet criteria to be admitted to the hospital. As I explored what had changed from her last visit, she suddenly shared that she felt an overwhelming, constant fear of dying at home alone. Every sensation of struggling to breathe or pain in her chest led her to believe that the end was near.
However, she didn’t fear her own death. She feared not being able to support other loved ones who had recently lost their jobs. The weight of her own illness and her family responsibilities had become nearly unbearable. Her eyes, as they welled with tears, silently pleaded with me for an absolution that I could not provide.

I started to take a step toward her from my place in the corner of the room to place my hand on her shoulder or arm in comfort, which is my usual practice. However now, I froze. My mind tried to make the impossible calculation about the increased risk of touching her despite my protective armor.
Another patient came to the ED for a standard complaint – injuries suffered during a fall in her home. However, our conversation quickly moved beyond her injuries, as she shared her difficulties in coping with the recent death of her terminally ill husband of over 50 years.
“I knew that he was going to die, but I always thought that I would be surrounded by my family and friends as I waded through this deep, dark grief…,” she uttered, as her voice trailed off.
The pandemic has brought me clarity on what my essential roles are as an emergency medicine physician and a member of our society.
I step into the hospital from a world where we are already isolated and physically distanced. Now in the ED, we are also hidden behind the physical barriers required to keep us safe – from the protective equipment like face masks to the use of technology, such as iPads, to communicate with patients in the room without entering. Despite the benefit of conserving scarce medical supplies and lowering exposure when possible, the use of iPads inevitably leaves my interactions feeling incomplete. Thus, every practitioner has been forced to navigate how and when to be physically present with the patient in the room and when to reach out a hand in comfort.
We can collectively rise from the pain, suffering and loss of this COVID-19 pandemic stronger than before. The pandemic has brought me clarity on what my essential roles are as an emergency medicine physician and a member of our society. Sometimes human connection is the best medicine that I can offer, and I often must create the space to look beyond the obvious to discover how I can truly strive to improve health and well-being. Similarly, there has never been a greater time to extend our hand, and we must broadly extend our collective hands to urgently address the larger, systemic issues harming health.
The only way that I can create the future I want to see is working one patient, and one day, at a time.
Renee N. Salas, MD, MPH, MS is an emergency medicine physician in the Center for Social Justice & Health Equity in the Department of Emergency Medicine at Massachusetts General Hospital, an assistant professor of Emergency Medicine at Harvard Medical School, a Yerby Fellow at the Center for Climate, Health, and the Global Environment at the Harvard T.H. Chan School of Public Health, and affiliated faculty and previous Burke Fellow at the Harvard Global Health Institute. Dr. Salas specializes in how the climate crisis is impacting health, clinical practice, the delivery of health care and public health.